Diabetic Foot
Introduction
Diabetes mellitus refers to a group of diseases that affect the way the body uses blood sugar (glucose). Glucose is an important source of energy for the cells that make up muscles and tissues. It is also the brain's primary fuel source. The main cause of diabetes varies depending on the type of diabetes each patient faces.
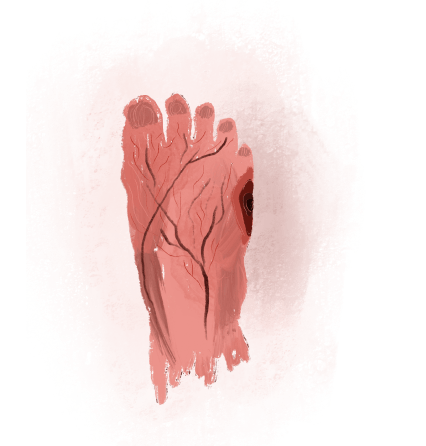
The diabetic foot constitutes a modern pandemic which is associated with the continuous increase of diabetics worldwide. By 2050 one in seven people is expected to be diabetic, while 25% of these patients will develop diabetic foot. The fact that every 20 seconds a diabetic foot is amputated somewhere on the planet highlights how dramatic the situation is and how important prevention and early treatment of it are.
What is a diabetic foot? How should people with diabetes take care of themselves and how can they avoid serious complications such as amputation?
Proper foot care, regular check-ups and correct management of diabetes can prevent problems before they become dangerous. If you notice changes in the skin, wounds that do not heal or unusual pain, do not hesitate to seek medical advice. For more information you can watch the video.

The timely early diagnosis of the disease
is very important
for the good outcome of the condition in both stages of the disease.
What is a diabetic foot?
The diabetic foot is the sum of the complications of diabetes in the tissues of the foot. Elevated sugar levels cause hardening and dehydration of the skin, changes in joint architecture (Charcot foot), inflammation of the bones (osteomyelitis), loss of pain sensation due to destruction of nerve fibers (neuropathy) and most importantly blockage of the small arteries of the foot (diabetic angiopathy). Consequently, the diabetic foot is a condition caused by the presence of angiopathy or neuropathy, conditions that disrupt blood circulation, slowing down wound healing. This results in minor injuries persisting, leading to infections, ulcers and gangrene.
Diabetic Foot: Symptoms
The appearance of symptoms in the diabetic foot depends in most cases on the type. The most important thing is for patients to recognize the early symptoms in a timely manner. Most frequently, patients with diabetic foot present with:
- Numbness, burning sensation or tingling in the toes and the sole of the foot
- Dry and hard skin, often with cracks
- Changes in the texture and color of the nails
- Small wounds that are slow to heal
- Darkening of a toe, which is an indication of reduced blood supply and possible development of gangrene
The timely diagnosis of the symptoms plays a decisive role in the prevention of serious complications. A wound on a diabetic foot is a sign that should not be ignored.
Ποιες είναι οι επεμβατικές μέθοδοι χειρουργικής θεραπείας;
How is the diabetic foot treated
There is not a single treatment option for the patient with diabetic foot, but a multidisciplinary approach by a specialized team of doctors. The patient with diabetic foot must be evaluated by a cardiologist, nephrologist and diabetologist in parallel with the vascular surgery assessment. Subsequently there should always follow a diagnostic angiography either with iodinated contrast agent (in patients with good renal function) or with carbon dioxide (in patients with renal insufficiency). Depending on the findings of the angiography and the results of the rest of the clinical examination, the best treatment is decided between the minimally invasive (endovascular) and open surgical method (bypass).
In our clinic, the full spectrum of the most complex vascular surgery conditions is performed through the modern Hybrid Clinic of the Athens Medical Center.
The role of the vascular surgeon
The Dr. Bisdas and the philosophy of our clinic holds one of the greatest experiences in Greece in the treatment of the diabetic foot with particularly low amputation rates. Our motto remains "NO TO AMPUTATION" and for this reason we have created a specialized team of doctors, nurses and podiatrists for the care of patients both during their hospitalization in the hospital and for post-operative home care. Furthermore our team offers the service of "SECOND OPINION" for patients who have been recommended amputation of the foot. In these patients we check whether all the necessary examinations have been performed that prove that a foot cannot be saved and in the event that it is technically feasible, we intervene to open the vessels and avoid major amputation. In a recent publication of ours, this strategy of ours led to more than 95% of patients avoiding amputation (Bisdas et al. Int J Low Extrem Wounds. 2022 Jun;21(2):174-181)!
Prevention and avoidance of amputation
Amputation is not the only option for patients with diabetic foot. Every patient with diabetic foot should undergo diagnostic angiography of the lower limbs before a decision for amputation is made. For this reason it is extremely important to seek a Second Opinionbefore reaching any final decision. However, in advanced and neglected cases, where there is irreversible damage or septic shock has occurred, amputation may be necessary. With proper prevention and care, these serious developments can largely be avoided.
Prevention is extremely important and is based on regular medical check-ups, good regulation of blood sugar and έγκαιρη αντιμετώπιση τυχόν προβλημάτων.
Do not ignore the symptoms! Early diagnosis can save your foot! For complete diagnosis and treatment Get in Contact with our clinic!
Frequently Asked Questions (FAQs)
What is a diabetic foot?
Diabetic foot is a serious complication of diabetes mellitus, which occurs when high sugar levels affect the nerves and vessels of the lower limbs. Neuropathy reduces the sensation of pain, while angiopathy limits proper blood supply. As a result, minor injuries can develop into serious wounds or ulcers.
What are the initial symptoms of diabetic foot?
In the initial stages, the patient may notice numbness, tingling or a burning sensation in the feet. Also, dry skin, changes in skin color and small wounds that do not close easily may appear. These signs are warning indicators of the risk of progression to ulcers.
How should a wound on a diabetic foot be treated?
Every wound on a diabetic foot is considered an emergency and requires immediate medical evaluation. The patient should not treat it alone with improvised methods, but should visit a doctor for cleaning, antisepsis and possible antibiotic treatment. Prompt intervention reduces the risk of infection and complications.
What happens if a diabetic foot develops inflammation?
Inflammation in the diabetic foot is dangerous because it can progress to infection of the tissues, even the bones. It is often accompanied by redness, swelling, pain and fluid discharge. If not treated in a timely manner, there is a serious risk of gangrene and amputation.
What medications are used for the treatment of diabetic foot?
The medication treatment depends on the severity of the problem. It usually includes antibiotics to combat infections and medications that improve circulation. At the same time, good regulation of blood sugar with antidiabetic medications or insulin is essential in order to support healing.
Which doctors specialize in the treatment of diabetic foot?
The care of diabetic foot is multidisciplinary. Diabetologists are involved for blood sugar regulation, vascular surgeons for the restoration of circulation and orthopedic or plastic surgeons for wound management. Specialized podiatrists also frequently participate for the prevention of injuries.
How is the diabetic foot treated?
The vascular surgeon plays a central role in the treatment of diabetic foot, focusing mainly on the restoration of blood circulation in the lower limbs. Through examinations he evaluates the condition of the vessels and, if he identifies stenoses or blockages, he can proceed with procedures such as balloon angioplasty/stent or surgical (by pass). The goal is the improvement of blood supply, which is of vital importance for wound healing and the avoidance of amputations.